You're here because someone—maybe a pediatrician, maybe a friend, maybe your kid's preschool teacher—told you to look into ABA therapy. And now you're drowning in contradictory information.
Some reviews say ABA changed their child's life. Others call it harmful. Some talk about 40-hour weeks and robotic drills. Others describe play-based sessions in living rooms.
So which is it?
I'm a BCBA who founded Achieving Stars Therapy after spending over a decade in this field—first as an RBT working sessions, then as a clinician designing programs, now running my own practice. I've seen ABA done beautifully. I've also seen it done terribly.
Here's what you actually need to know.
What the Research Says About ABA Therapy Effectiveness
Let's start with data, not opinions.
The Lovaas Study (1987): Dr. O. Ivar Lovaas tracked kids through intensive ABA therapy. Results? 90% showed significant improvement. This is the study everyone cites. But here's what they don't tell you: "intensive" meant 40 hours per week. With 1960s methods. Using punishment alongside rewards.
That's not how modern ABA works.
Recent Meta-Analysis (Virués-Ortega, 2010): Analyzed multiple studies and found ABA therapy improved outcomes across seven of eight measured areas—cognitive, language, social/communication, problem behavior, adaptive behavior, emotional, and autism symptoms.
The catch: Most studies don't measure Quality of Life. They measure behaviors. There's a difference.
Modern Dosage Studies (Mece & Sherifi, 2022): Tracked a child receiving just 4.5 hours per week of play-based ABA for three years. Results? Better engagement with other kids. More imitation of sounds and actions. Way more communication and actual language.
Translation: You don't need 40 hours a week. You need the right approach.
Real Parent Reviews: What Actually Changes
Forget the clinical studies for a minute. Here's what parents tell me changes when ABA therapy works:
"Her meltdowns used to last 45 minutes. Now they last 5. And she can tell us what's wrong instead of just screaming."
— Denver mom (11 months of therapy)"He asked for a snack with words. No screaming. No pulling me to the pantry. Just 'crackers please.' I cried."
— Colorado Springs dad (8 months of therapy)"She asked 'why?' for the first time. Not echolalia. A real question. About why the sky is blue."
— Boulder mom (14 months of therapy)Notice what they're NOT saying? They're not saying their kid is "cured" or "normal now." They're saying life got easier. Communication improved. Meltdowns became manageable.
That's what good ABA does.
The Controversy: Why Some People Hate ABA Therapy
Let's talk about the elephant in the room.
ABA therapy has legitimate critics. And some of that criticism is justified.
Historical ABA (1960s-1990s):
- Used punishment alongside rewards
- Focused on eliminating "autistic behaviors" rather than building skills
- Pushed 40-hour weeks with rigid drills
- Tried to make autistic kids appear "normal"
Why that was harmful:
It treated autism as something to fix rather than a neurological difference to support. It suppressed self-soothing behaviors (stimming) that weren't actually problems. It exhausted kids.
Modern ABA (2020s):
- No punishment. Period.
- Focuses on skill-building, not behavior elimination
- Play-based and naturalistic
- 10-25 hours per week (not 40)
- Respects neurodiversity while teaching functional skills
The field evolved. Not every provider evolved with it.
What Makes Good ABA Therapy: Red and Green Flags
After a decade in this field, here's how I tell parents to evaluate providers:
🚩 Red Flags (Run Away):
That's not the goal. The goal is skill-building.
That's outdated and exhausting.
These aren't problems to fix.
Huge red flag. Transparency matters.
You should understand the science, not just follow orders.
Quality control matters. Period.
Modern ABA uses natural, varied reinforcement—praise, access to preferred activities, not just goldfish crackers.
✅ Green Flags (Keep Investigating):
Parent input should drive the treatment plan, not some cookie-cutter curriculum.
Naturalistic teaching works way better than drills at a table.
You should see measurable progress. Actual graphs. Real numbers.
Someone with a master's degree should be watching sessions regularly, not once a quarter.
Caregiver coaching means progress continues when the therapist leaves.
No miracle promises. No "your child will be indistinguishable from peers" nonsense.
You can tell the difference between someone going through the motions and someone who actually enjoys being there. Personality fit matters way more than credentials.
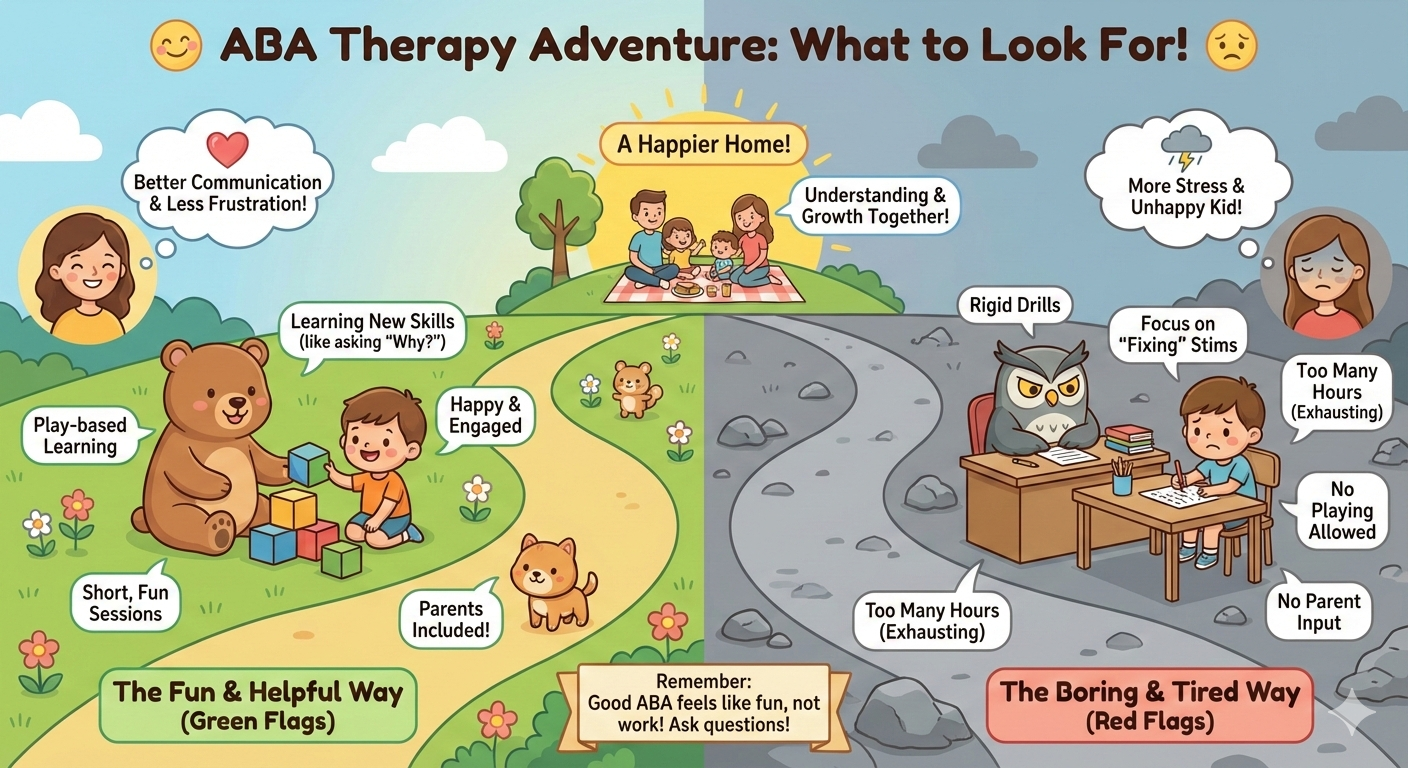
Modern ABA (left path) vs. Outdated ABA (right path) - Choose the path that leads to a happier home!
How to Choose an ABA Provider: The Research-Backed Approach
Step 1: Verify Credentials
Every provider should have:
- BCBA: Board Certified Behavior Analyst (master's-level clinician)
- RBT: Registered Behavior Technician (direct therapist)
- BACB: Behavior Analyst Certification Board oversight
- State licensure (Colorado, Ohio, Kansas, New Hampshire, New Jersey)
In Colorado, for example, all ABA providers are required to be licensed. Most aren't. That tells you something about their commitment to quality.
Step 2: Ask About Their Approach
Questions to ask:
- "How many hours per week do you typically recommend?" (10-25 is reasonable)
- "What does a typical session look like?" (Should sound like play, not drills)
- "How often will the BCBA supervise sessions?" (Weekly minimum at start)
- "What's your philosophy on stimming?" (Should respect self-soothing behaviors)
- "Can I observe sessions?" (Answer should be yes)
Step 3: Check Insurance and Medicaid Coverage
Colorado Medicaid covers ABA therapy. So does most private insurance. If a provider says "we don't take insurance," that's a red flag. Good providers handle authorization.
Step 4: Trust Your Gut
If something feels off, it probably is. You know your kid better than anyone.
Where Achieving Stars Therapy Fits: An Honest Assessment
I'm obviously biased—I founded this company. But here's how we approach ABA differently:
What we do:
- 100% in-home therapy (no centers, no waiting rooms)
- Play-based, naturalistic approach
- 10-25 hours per week (not 40)
- Weekly BCBA supervision
- Colorado Medicaid + most insurance accepted
- We switch RBTs if personality fit doesn't work
What we don't do:
- We don't promise to "cure" autism
- We don't focus on eliminating harmless stims
- We don't use punishment
- We don't run 40-hour programs
- We don't force eye contact or "quiet hands"
Why in-home matters (according to research): Kids generalize skills better when they learn them in their natural environment. A 2022 study found that in-home ABA led to faster skill acquisition because children practiced in the contexts where they'd actually use those skills—their own kitchen, their own bathroom, their own playroom.
Our outcomes data:
We're not perfect. No provider is. But we're transparent about our approach, our data, and our limitations.
What ABA Therapy Can and Can't Do
ABA therapy CAN help with:
- Communication (requesting, protesting, conversational skills)
- Daily living skills (toileting, dressing, hygiene)
- Social skills (turn-taking, sharing, reading social cues)
- Challenging behaviors (understanding WHY, teaching replacement skills)
- School readiness (following directions, sitting for activities)
ABA therapy CANNOT:
- "Cure" autism (that's not the goal)
- Make your child neurotypical (nor should it try)
- Work overnight (progress takes months, not weeks)
- Replace medical interventions (it's behavioral, not medical)
- Fix everything (some challenges persist regardless)
The Cost Question: What Parents Actually Pay
With Colorado Medicaid: $0 out-of-pocket
With private insurance: Usually $0-50 per session (depending on copay/deductible)
Without insurance: $50-150 per hour
- RBT sessions: $50-80/hour
- BCBA sessions: $100-150/hour
Total monthly cost (uninsured): $2,000-6,000 depending on hours
That's why insurance matters. Good providers handle the authorization paperwork so you don't have to fight with insurance companies.
How to Tell If It's Working: Progress Markers
First 3 months: You should see some change. Maybe transitions are easier. Maybe meltdowns are shorter. Maybe your kid is using more words.
6 months: You should see noticeable improvements in whatever skills you're targeting. Your BCBA better be showing you data graphs, not just saying "he's doing great."
12 months: Significant progress in at least 2-3 major areas. And honestly? Family stress should be going down. If you're still as overwhelmed as when you started, something's not working.
If you're NOT seeing progress after 6 months: Either the approach needs adjusting or the provider isn't the right fit. Don't fall into the trap of "let's just give it more time." Six months is enough data to know if it's working.
The Bottom Line: Is ABA Therapy Worth It?
Here's what I tell parents in consultations:
ABA therapy works when:
- You have a good provider who uses modern, play-based methods
- Your child receives adequate hours (10-25/week, not 40)
- You're involved in learning the strategies
- Goals focus on functional skills, not "looking normal"
- Progress is measured consistently
ABA therapy doesn't work when:
- Provider uses outdated methods (rigid drills, punishment)
- Hours are too low (2-3/week isn't enough)
- RBT and child don't click (personality fit matters)
- Goals focus on eliminating harmless behaviors
- There's no BCBA supervision
Is it worth it? For most families, yes. But only if you find the right provider.
Next Steps: Starting ABA Therapy the Right Way
- Get a formal diagnosis first. Insurance won't cover ABA without it. You need an official autism diagnosis from a licensed psychologist or developmental pediatrician.
- Contact 2-3 providers. Don't just go with the first one. Compare their approaches. See who actually answers your questions.
- Ask the questions from this article. Evaluate how they respond. If they get defensive or dodge questions, that tells you something.
- Observe a session. See their methods in action. Watch how the therapist interacts with kids. If they won't let you observe, run.
- Check your insurance coverage. Get benefits verified before you commit. Good providers will do this for you within 48 hours.
- Trust your gut. If something feels off during that initial consultation, listen to that feeling. You know your kid better than anyone.
If you're in Colorado, Kansas, Ohio, New Hampshire, or New Jersey, we'd be happy to talk. No sales pitch—just real information about whether in-home ABA makes sense for your family.
Frequently Asked Questions About ABA Therapy Reviews
How do I know if ABA therapy reviews are real?
Look for specific details. Real reviews mention actual progress—stuff like "transitions got easier" or "he's using 3-word phrases now." Fake reviews just say "therapy is great!" with zero specifics. Check Google reviews, therapist platforms like Psychology Today, and ask the provider for parent references you can actually call.
What's a realistic timeline for seeing results?
Most families notice some improvement within 3 months. Maybe meltdowns are shorter. Maybe your kid is using a few more words. Real significant changes? Usually shows up around 6-12 months. If you see absolutely nothing after 6 months, time to reassess the approach.
Should I try ABA therapy even with mixed reviews?
Mixed reviews usually mean different approaches. The center-based provider doing 1960s drills gets awful reviews. The in-home provider using play-based methods gets great ones. Ask providers exactly what their approach looks like.
How many hours per week do most parents report as effective?
The sweet spot seems to be 10-25 hours per week. Less than 10? Progress is really slow. More than 25? Kid gets exhausted and burnt out.
What do negative ABA therapy reviews usually complain about?
Common complaints: rigid drills, focus on eliminating stims, excessive hours, lack of BCBA supervision, poor communication. These are provider problems, not ABA problems.
Ready to Learn More?
We provide BCBA-supervised, in-home ABA therapy that respects your child's neurodiversity while building functional skills.
Call: (833) 666-3115
Email: [email protected]
Fax: (833) 666-1401
Call